Human papillomavirus (HPV) is the collective name for a group of DNA viruses that are spread from person to person and provoke the development of benign neoplasms - papillomas. Some varieties are oncogenic (i. e. , they increase the risk of malignant tumors). HPV is most often associated with cervical cancer, which kills thousands of women worldwide each year. However, the virus also affects the development of other cancers: not only in women, but also in men.
HPV does not manifest itself as a symptom for a long time: patients often find out about it only when a precancerous or cancerous condition develops. HPV is a threat to patients of any gender and age, including young children. But, the main "target audience" is 15-30 year olds: they are sexually active, do not always think of precautions, and in most cases HPV is sexually transmitted.
To prevent the effects of the virus on the body so far, it is recommended to check your health status regularly: to exclude pathologies that can cause it. There are also tests for HPV to detect the presence of oncogenic strains. Take care of your health now: make an appointment at Otradnoe Polyclinic and visit a doctor without having to wait in line or adjust to uncomfortable times for you
What is HPV
Human papillomavirus, entering the body through the skin microtraum, is introduced into the epithelial lining cells. HPV can exist in any layer of the epidermis. However, its reproduction occurs exclusively in the basal layer.
Viral development occurs in 2 stages:
- Reproductive - the virus enters the cell without affecting its chromosomes, and reproduces.
- Integrative - HPV is introduced into the genome of infected cells.
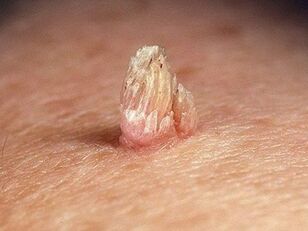
In the second stage the virus changes cells. They begin to actively divide, and tumor-like formations - papillomas - appear. This is a prominent papillary growth on the surface of the skin (which is why it is called: papilloma - from the Latin papilla - nipple and oma - Greek tumor). The second stage is not always the case. This virus, which is in the first stage of development, can retreat (leaving the body). However, even if the patient does not experience pathological changes, he or she is a carrier of HPV and is capable of infecting others.
The incubation period can last from 3 weeks to a year. On average, it is 3 months. In some cases, non-genital papilloma forms first appear, and then neoplasms appear on the genitals.
In most cases, the body overcomes the virus within 2 years. However, re-infection can occur - with the same or different strains. Also, papillomas or other skin manifestations can deteriorate after 6-8 months (gradually decreasing and then disappearing). This occurs when the immune system suppresses the virus and "survives" from the cell.
HPV virus most often affects skin and mucous membranes:
- Anogenital area.
- Upper respiratory tract.
- Mouth cavity.
- Bronchus.
- Connection.
- Rectum.
- Esophagus.
Type HPV
The first human papilloma virus (HPV) was isolated in 1971. And scientist Harald zur Hausen was able to identify and prove the link between HPV and cervical cancer. After that, he received the Nobel Prize for his discovery.
About 600 different HPV strains are known to date. Some provoke the appearance of warts, others - genital warts, and others - papillomas. There are also types among HPV that affect the development of cancerous tumors. They are called oncogenic. Fortunately, not many of them. They can have low, medium or high oncogenic potential:
- Strain 6, 11, 40, 42, 43, 44, 54, 61, 70, 72, 81 are characterized by low oncogenicity.
- Oncogenic averages of types 26, 31, 33, 35, 51, 52, 53, 58, 66.
- High oncogenic potential in strains 16, 18, 39, 45, 56, 59, 68, 73, 82.
Cervical cancer is mostly caused by types 16 and 18.
Help!The presence of oncogenic HPV type in the body does not mean that a person is "punished" for cancer. The presence of the virus increases the risk of getting cancer, but it is not the only cause of its occurrence.If a patient has an oncogenic HPV strain, he or she should only monitor his or her health on a regular basis, regularly undergoing preventive screening. If necessary, the doctor will prescribe the appropriate therapy for him.
Female and male reproductive systems can infect about 40 types of papillomavirus. The result of their activity is not only cancer, but also genital warts or condyloma.
Help!Cancer tumors grow slowly: within 5-30 years after being infected with the papillomavirus virus. They are preceded by a precancerous condition (benign neoplasms that can degenerate into malignant). That is why it is very important to have regular preventive checkups. And precancerous conditions, even cancer in the early stages can be treated perfectly, and dangerous consequences can be avoided.
HPV transmission route
The main "condition" of infection is the presence of micro-damage (cuts, cracks, scratches) on the skin or mucous membranes. They are the "gateway" to HPV.
Often, viral transmission occurs when the skin or mucous membranes of two people come in contact. Thus, the main route of papillomavirus is sexual intercourse. Moreover, the use of condoms does not exclude the possibility of infection. The virus can be transmitted through oral sex, where contraception is not always used. In addition, condoms do not cover the entire surface of the penis, and are often worn in the middle of sexual intercourse. HPV can also be contracted by kissing.
HPV can also be transmitted:
- From mother to child as the baby passes through the birth canal.
- At home: while using other people's hygiene products (towels, toothbrushes, shaving accessories).
- In public: sauna, gym, swimming pool.
Help!The duration of papillomavirus survival in the external environment is short. Thus, the risk of domestic infection, although available, is much lower than sexual intercourse.
Self-infection may also occur: virus transmission from one part of the body to another during shrinkage, scratching the skin, biting the nail.
Virus infection does not occur in all cases. The following factors increase risk:
- Decreases immunity.
- Bad habits: smoking, alcohol abuse.
- Pressure.
- Sexually transmitted infections.
- Urinary tract disease.
- Injuries to the skin and mucous membranes.
- Immune deficiency condition.
- Long-term use of hormonal contraceptives.
Help!Oncogenic HPV strains are more dangerous for women than men, as they are more often infected.
HPV: symptoms
Papillomavirus has no symptoms for a long time. Usually, patients are aware of the presence of HPV with the development of its consequences: the appearance of warts, papillomas, genital warts. In some cases, the following signs may indicate a virus:
- Redness, skin growth (most often in the genital area);
- Itching.
- Pain and other discomfort during or after intercourse.
What diseases can HPV cause?
Papillomavirus, first of all, provokes the growth of papillomas, warts and genital warts in patients of both sexes. All of the above neoplasms can occur on any part of the body. However, it often affects the genitals and anal area. In women, they occur in the vulva, cervix, and vagina. In men - scrotum, penis head, foreskin. In patients of both sexes, neoplasms often appear in the anus.
Also, warts often appear on the soles of the feet, larynx, vocal cords. Papillomas (flesh-colored papillomas) do not have a "favorite spot" - they can appear on the trunk, neck, face, arms and legs. In children and adolescents, flat warts are most common (they are also called youthful or adolescent). This is a small dark neoplasm (3-5 mm) that protrudes slightly above the surface of the skin. Often it occurs on the back of the hands, face, feet.
Regarding cancer, most patients are associated with HPV, first of all, cervical cancer. Indeed, this pathology is very common in our time. However, in women, HPV also often provokes the development of vaginal and vulva cancer (65-70% of cases), in men - penile cancer (50% of cases). Also in women and men, papillomavirus can contribute to the occurrence of malignant tumors:
- rectum;
- oral cavity;
- larinks.
In children, HPV, as a rule, is indicated by the growth of papilloma against the background of decreased immunity due to previous diseases, usually viral or bacterial infections. Also, papillomavirus infects young patients with frequent allergic reactions or colds.
HPV and pregnancy
Papillomavirus negatively affects female fertility. If present, the likelihood of pregnancy will be doubled, as HPV can interfere with the cultivation of fertilized eggs. If the couple is also infected with the virus (which occurs in 65-70% of cases), then the chances of fertilization are reduced. HPV has a negative effect on sperm motility.
During pregnancy, papillomavirus increases the risk of infection:
- Few or polyhydramnios.
- Chronic placental abruption.
- HPV can also cause miscarriage.
Therefore, pregnant women are prescribed drug therapy that can reduce all of the above risks.
When a child passes through the birth canal, there is a risk of infection. Therefore, women with HPV are better able to give birth with caesarean section - the risk of viral transmission is reduced by 5 times.
Hormonal background changes provoke rapid growth of genital warts. They can grow together, which can cause difficulty during urination and defecation, giving an unpleasant sensation when walking, bleeding. During childbirth, neoplasms are easily injured. They also make it difficult for the baby to go through the birth canal. To avoid all this, genital warts are treated early in pregnancy. Methods such as cryodestruction, laser surgery, etc. are used.
Diagnostics
To diagnose HPV, they first see a doctor. Depending on the manifestation of the virus, he or she will refer the patient to a diagnostic study and to a narrow specialist (gynecologist, urologist, dermatologist, oncologist, proctologist, etc. )
Both women and men can be given exams such as:
- ELISA blood test - according to the results, it is impossible to determine the concentration and oncogenicity of the virus, but antibodies to it can be detected, this method is very suitable for early diagnosis, when symptoms have not yet appeared.
- PCR diagnostics - allows you to detect HPV DNA, which allows you to know exactly whether there is a virus in the body or not; blood, saliva, discharge from the genitals, etc. are taken for analysis.
- Digene test - allows you to assess the level of strain toxicity, to determine the amount of virus in the body; A biomaterial is a piece of tissue, scraping from the cervical, vaginal or urethral ducts.
Women are prescribed the following types of examinations:
- Cytological examination (PAP test) - smear examination of the vagina under a microscope to identify virus-modified cells.
- Colposcopy - cervical examination using a colposcopy device, this procedure is prescribed to the patient if the modified cells are found in accordance with the results of cytological examination.
Treatment
There is no specific treatment for HPV (which aims to eradicate it). However, you can take steps to suppress viral activity and increase the likelihood of self-healing. Patient prescribed:
- Vitamins.
- Immunomodulator.
- Antivirus drugs.
Symptomatic treatment is also performed - neoplasm removal. Never try to treat condyloma, papilloma and warts with folk remedies. There is a risk of provoking the development of secondary infections or degeneration of benign tumors into malignant tumors.
The following methods are used to get rid of neoplasms:
- Removal with a scalpel.
- Cryodestruction (freezing with liquid nitrogen).
- Removal with a radio knife.
- Laser removal.
- Electrocoagulation.
This method is chosen by the doctor depending on the nature and location of the neoplasm, as well as the condition of the patient's body.
Prevention

Preventive measures include maintaining a healthy lifestyle and periodically strengthening immunity with the help of a full and varied diet, moderate physical activity, and quality rest. It is important to follow the rules of personal hygiene, do not use other people's accessories. To avoid the risk of infection, you should refrain from regular sexual intercourse and use barrier contraception.
Currently there is also the possibility of vaccination against some highly oncogenic HPV strains. Vaccination is recommended between the ages of 9 and 26 years (optimum age is 11-12 years). Women can be vaccinated after 26 years, but only if the gynecologist believes that there is evidence. Keep in mind that vaccination does not cure the virus already in the body, but prevents infection with some of its most dangerous types.























